A SMALL PLAQUE hanging in the home of Randy and Ellen Layne contains a familiar saying: “Love is patient. Love is kind. Hopes all things. Endures all things. LOVE NEVER FAILS.”

A plaque that hangs in the Laynes’ Crystal Lake, Illinois, home represents the couples’ devotion to each other. Photo by Martha Irvine
It’s a biblical passage so often quoted—at weddings, on anniversary cards—that one could breeze past this little ceramic wall decoration and hardly take notice. In the Laynes’ home in suburban Chicago, however, it quickly becomes apparent that those words have held true through two decades of marriage, especially since Randy was diagnosed with bladder cancer in 2006.
“We’ve always been best friends,” says Randy, 55, whose favorite morning ritual includes rising early to drink coffee, read the newspaper and chat with his wife. “I’d just as soon do something with her as anybody else.”
The Laynes’ long-standing friendship began when the couple met while working at a savings and loan association in Phoenix. They married in 1994 and became a family with her 6-year-old son from a previous marriage, Cory Shier. Their son, Hunter, was born the following year.
Time together has become more plentiful since Hunter, 19, went away to college in August 2014, leaving only their faithful chocolate lab, Sparky, to keep them company. It’s given the empty nesters a chance to reflect on Randy’s diagnosis and recovery.
“For us, it was a whirlwind,” Ellen says, one with effects that still linger.
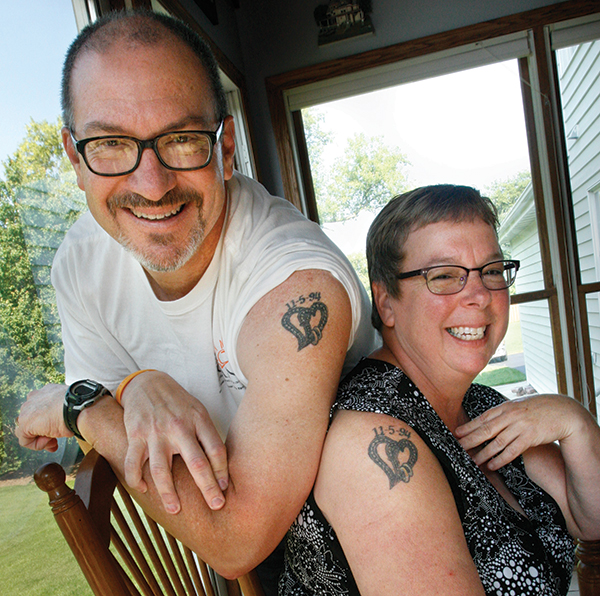
Randy and Ellen Layne got matching tattoos with their wedding date to celebrate their 15th anniversary in 2009. Ellen has been at Randy’s side throughout his experiences with bladder cancer. Photo by Martha Irvine
Getting Through a Busy Time
Bladder cancer is the sixth most common cancer in the United States—about 75,000 new cases are diagnosed each year. But before his diagnosis, Randy had never heard of the disease. He was only 46 when a doctor first mentioned the possibility that he had bladder cancer, much younger than the usual bladder cancer patients, who most often are diagnosed in their 60s or 70s. An executive in the mortgage industry, he’d moved to Crystal Lake, Illinois, a suburb northwest of Chicago, in November 2005, from the Washington, D.C., area.
Randy’s only symptom, blood in his urine, appeared in December after he’d been sledding with Hunter, then 10. He had hit his back on a tree, so he assumed the blood was related to that and went to the emergency room. The ER doctor prescribed an antibiotic and told him to follow up with his family doctor if the blood appeared again, which it did in 2006. Randy saw his primary care physician. There were no other symptoms—a red flag to the doctor, whose own mother had died recently from bladder cancer.
Randy recalls the doctor saying, “Now, not to alarm you, but I’m going to send you to the urologist.” The urologist saw, in a CT scan, a diverticulum, a pouch in the bladder that can be congenital or develop later in life. But the doctor didn’t discover the tumor inside the diverticulum until the blood in Randy’s urine appeared more frequently, prompting a cystoscopy in fall 2006. A cystoscope is a flexible instrument passed through the urethra directly into the bladder that the doctor can use to look for and, if needed, remove small tumors. In Randy’s case, the doctor found a 1.5-centimeter tumor that was eventually classified as a T2a tumor, meaning the cancer had grown into the inner half of the bladder’s muscle layer.
It was a hectic period in Randy’s life. He had just traveled to New Mexico to bring his elderly parents’ belongings to Illinois, where they eventually moved into an assisted-living facility near his home. One week after his parents arrived in October 2006, he received the bladder cancer diagnosis.
The urologist suggested he see a doctor with more experience treating bladder cancer, so he went to Christopher L. Coogan, a urologic oncologist at Rush University Medical Center in Chicago. Coogan says he was concerned that the cancer might be muscle invasive because of the tumor’s appearance.
About 26,250 of the roughly 75,000 people who are diagnosed with bladder cancer each year in the U.S. have cancer that has invaded the deeper layers of the bladder, according to the American Cancer Society. Tumors that have not invaded the muscle can be treated with chemotherapy and removed endoscopically. But Randy’s case was advanced enough that Coogan recommended a nerve-sparing radical cystectomy. He removed Randy’s bladder and replaced it with a neobladder constructed with a portion of his small intestine. This has given him the ability to urinate in the usual way, without using a catheter or urine bag worn outside the body. Before the surgery, Coogan also addressed with Randy the possibility of erectile dysfunction, a common side effect when the bladder is removed—and one that can sometimes be rectified with drugs or a penile implant after surgery. Whatever the outcome, they agreed to focus on saving Randy’s life.
Through all of these conversations, Ellen was Randy’s constant companion, his rock—including that November day in 2006 when she nervously waited seven hours for his surgery to end. When she first went in to see him with her sister, a former nurse who is now a hospital administrator, Randy looked up at them.
“I made it,” he said in a weak voice, and that was all.
Ellen remembers walking out of the room, out of Randy’s sight, and bursting into tears.
“I was so shocked at how he looked. He looked horrible,” she says.
Smoking isn’t just associated with lung cancer.
Most people associate smoking with lung cancer, but experts say few people know that smoking is also the single greatest risk factor for bladder cancer. A study published in 2006 in the Journal of Urology surveyed patients at a urology clinic to determine how much they knew about the risk factors for bladder cancer. They also were asked about their own smoking habits.
Of the 280 patients who completed the survey, 98 percent stated that smoking was a risk factor for lung cancer. But only 36 percent thought smoking was a risk factor for bladder cancer.
“Our study suggests the need for the American public to be better educated to help combat smoking-related cancers,” the study’s authors concluded.
Christopher L. Coogan, a urologic oncologist at Rush University Medical Center in Chicago, treats many bladder cancer patients in his practice. He says the lack of awareness of the link between smoking and bladder cancer is sobering.
“You are two to six times more likely to get bladder cancer if you smoke. So with a decrease in smoking, you’d likely see a decrease in bladder cancer,” he says, citing data from several studies that examined the link between smoking and bladder cancer.
In fact, he believes that cutting the number of smokers is “the biggest thing we can do” to reduce the incidence of bladder cancer.
A Difficult Recovery
Hunter, then 11, visited his father in the hospital once, but couldn’t stand seeing him with a large incision and tubes on either side to drain urine until the neobladder functioned fully.
“No one wants to see a loved one having that many tubes coming out of them,” Hunter says now.
After 10 days in the hospital, Randy went home, though he had to be readmitted shortly after for a small bowel obstruction, a common complication managed by slowly easing a patient back onto solid foods, Coogan says.
Randy finally returned home for good on Dec. 1, 2006—only to have his elderly mother rushed to the hospital that same night for emergency surgery to have a tumor in her colon removed. She pulled through initially but died of kidney failure in May 2007 at the age of 84.
Somehow, with gentle but firm nudging from Ellen and fueled by his own wish to recover, Randy found the motivation to get better, returning to work after just two months off. But he had lost 30 pounds and didn’t have much strength or energy.
“It’s a big deal. It takes a toll on you,” Randy says of his treatment and recovery.
By spring 2007, he felt well enough to return to coaching youth baseball. But he told very few people about the cancer, unless they commented on his frequent trips to the bathroom or asked why he was only having a couple of beers. (Alcohol only increases those trips to the bathroom.)
“It’s not like it was a secret,” Ellen says.
“No, it’s just not something … ,” Randy continues, then pauses.
“It’s just an awkward conversation to come up, I guess,” Ellen says.
Over time, Randy adjusted to the neobladder. He had started doing Kegel exercises before the surgery to strengthen his pelvic floor muscles and still does at least 100 every day to help him control the neobladder, which he knows is full when he feels pressure in his lower abdomen.
Eight years after the surgery, he has had some minor scares. In 2013, for instance, he was having trouble urinating and thought his neobladder had stopped working. But it turned out a stone was blocking the urethra. Coogan was able to crush the stone and remove the bulk of it through a scope during an office visit. Then Randy passed what remained of the stone in his urine.
Now that Randy is three years beyond the five-year benchmark since diagnosis, Coogan is hopeful about his patient’s progress, but he says checkups will continue annually. As he told Randy when they first met, “We’ll be together the rest of your life.” That may be true, unless Randy finds a new doctor in Ohio, where he accepted a job at a mortgage company based in Wilmington. He started there in August 2014.

Randy Layne speaks at a 2013 think tank sponsored by the Bladder Cancer Advocacy Network in Snowmass Village, Colorado. Photo courtesy of the Bladder Cancer Advocacy Network
Reaching Out to Help Others
Since his surgery, Randy has dedicated time to volunteering for the Bladder Cancer Advocacy Network (BCAN), a nonprofit organization that promotes bladder cancer awareness and research.
“It’s not a lot, but I do what I can,” he says. “Having made it through this myself, if I can do something to help others, I feel like I ought to do that.”
Randy was a patient representative on a U.S. Food and Drug Administration (FDA) advisory committee that, in December 2009, recommended approval of blue light cystoscopy, an enhanced imaging technique that allows a more accurate diagnosis of bladder cancer by making tumors easier to see. The FDA approved the technology in 2010. With BCAN, Randy has lobbied members of Congress about additional funding for bladder cancer research, which Randy and BCAN organizers say has received less funding than research for higher-profile cancers. On a more personal level, he’s taken time to speak by phone with newly diagnosed bladder cancer patients to answer their questions and offer his support.
“I adore him. He’s a wonderful person and very honest and direct—and there’s a special spot in my heart for him because he’s one of the first volunteers we had,” says Diane Zipursky Quale, who co-founded BCAN in 2005 with her husband, John Quale, who had bladder cancer.
Before John’s death in 2008, he and Randy had candid conversations, including about their experiences with sexual dysfunction—a source of turmoil for Randy since the surgery. In 2013, Randy spoke at a BCAN think tank panel, where he told doctors about his struggles and advised them to take more time to explain the potential for long-term sexual dysfunction to new patients. His work with BCAN has helped him work through these and other issues, he says, as has the passage of time. Still, the question “Why me?” is inevitable.
He never smoked, a big risk factor for bladder cancer. But his father, a former aircraft mechanic, was a heavy smoker and died in 2012 when lung cancer metastasized to his brain.
“Back in the ’60s and ’70s, you made long car trips with the windows rolled up and people smoking. Put two and two together, as far as I’m concerned you could … ,” he pauses and throws up his hands.
Randy admits that he still feels an underlying anger that surfaces from time to time, sometimes over something as silly as a wrench dropped in the garage, his wife says.
“You know those people who are like, ‘I beat cancer … and my life is wonderful. I’m just happy. I’m happy to be alive. I’m happy, happy, happy’?” Ellen says, as her eyes moisten with tears. “That was not Randy. And my expectation of him was …”
“To be like that,” Randy says, finishing her sentence as they often do for one another.
He is extremely grateful, Randy insists. He and Ellen have gone to counseling, individually and as a couple at their most difficult points. And he says he is more ready than ever to talk about his cancer and the impact it’s had, especially since he has struggled with bouts of depression in recent years. Among other things, he says he is still processing the grief he feels over not spending more time with his mother because of his own illness. Then there is the sexual dysfunction and failed attempts to find a solution.
Being more open has helped, Randy says. In fall 2013, he did an interview with a local newspaper, telling them about his bladder cancer and his lobbying trip to Washington with BCAN.
At home, he assures his wife that, with more time together as a couple, they can revisit his sexual dysfunction.
“Now we can work on it,” he tells her.
“Yeah, exactly. So that’s kind of an exciting thing,” Ellen says, her eyes brightening. “I mean, have you ever thought about that? Because I have.”
“Yeah, absolutely,” Randy says. Then he teases her, “No, no, never gave it another thought.”
They laugh, and there is a sense of comfort in believing that, no matter what happens, they’ll forge ahead, together.
“You go on with your life,” he says, “and you try to be as normal as you can.”
Cancer Today magazine is free to cancer patients, survivors and caregivers who live in the U.S. Subscribe here to receive four issues per year.





