AS A NURSE, Brenda Oehler knew about the possible side effects of her chemotherapy treatments. Oehler, the director of nursing operations at UnityPoint Health – St. Luke’s Hospital in Cedar Rapids, Iowa, was diagnosed with stage II lobular breast cancer in March 2021. “I expected to lose my hair and to be tired,” Oehler says.
When she started chemotherapy that April to reduce the size of her tumors and treat suspicious lymph nodes before surgery, her health care team told her about the possibility of developing peripheral neuropathy, nerve-related symptoms in the hands and feet resulting from chemotherapy. But she was in her late 40s—still shuttling kids to and from their activities and walking every day—and she handled her chemo treatments, a combination of doxorubicin and paclitaxel, much better than she imagined. “I really didn’t think it would impact me,” she says.
About three months into her chemo treatments, however, in July 2021, Oehler noticed she was having trouble walking. It felt like she was wearing socks all the time, even when she was barefoot. “I couldn’t always tell when my foot was touching the ground,” she says. “I was tripping over the carpet at times.” At work, she had to switch from the dressy shoes she loved to sneakers.
After her chemo treatments ended in August and she underwent a double mastectomy that September, the numbness continued to affect her. She fell while on a treadmill and began to feel helpless. “I felt like it was really limiting me,” she says of the neuropathy.
Chemotherapy drugs that are used to treat cancer can have many side effects, from hair loss to nausea. But several of the drugs can also cause peripheral neuropathy, a side effect that can linger long after treatment has ended. Certain chemotherapies are known for their link to neuropathy, including taxanes often used to treat breast cancer. Paclitaxel, the taxane that was part of Oehler’s treatment, “is a big offender,” says Charles Loprinzi, a medical oncologist at Mayo Clinic in Rochester, Minnesota, who has studied the side effects of cancer treatments for more than three decades. Other chemotherapy drugs known to cause neuropathy include platinum-based compounds like oxaliplatin, often used to treat colorectal cancer patients.
The pain, numbness and tingling brought on by neuropathy can be debilitating. One of the greatest challenges, Loprinzi says, is that “a lot of things have been tried and nothing has been proven to work to prevent the neuropathy from happening.” And once peripheral neuropathy occurs, he says, “we don’t have a lot of good drugs for treating it.” One drug is the antidepressant duloxetine, which neuropathy guidelines from the American Society of Clinical Oncology (ASCO) indicate could be useful in treating neuropathy, although more research is needed.
The lack of effective treatment options can mean that, for some patients, the tingling, burning or shooting pain associated with neuropathy might require the health care team to adjust, or even stop, chemotherapy treatment. Yet there is hope for several promising interventions—from exercise to acupuncture—that some people with cancer have found helpful in treating their neuropathy once it starts. Along with testing these techniques to see if and how they could become a part of standard treatment guidelines for neuropathy, researchers like Loprinzi are running clinical trials of treatments such as cryotherapy and compression therapy to determine whether they can stop neuropathy from happening in the first place.
A Far-reaching Problem
Chemotherapy-induced peripheral neuropathy (CIPN) affects many patients who receive chemotherapy. More effective treatments, from newer chemotherapies to immunotherapy, have made it possible for more people to recover after a cancer diagnosis. But peripheral neuropathy can make it difficult to thrive. While neuropathy symptoms can resolve once treatment ends or in the months that follow, Loprinzi says, “it can continue to be a chronic problem for years and a very bothersome problem for some patients.” Studies suggest that more than two-thirds of patients undergoing chemotherapy will experience some level of peripheral neuropathy one month after chemotherapy, dropping to about 30% of patients still experiencing this side effect after six months.
Researchers are interested in learning who is at the greatest risk for peripheral neuropathy so they can possibly tailor treatments to the patients’ needs and be ready with a plan if neuropathy symptoms emerge. Known risk factors for CIPN include previously existing neuropathy, conditions linked to nerve damage such as diabetes and older age, and the number of chemotherapy cycles received.

Photo by PeopleImages.com – Yuri A / Shutterstock.com
To better tailor chemotherapy for individual patients with the goal of maximizing treatment efficacy and minimizing toxicity, Meghna Trivedi, a breast oncologist at Columbia University Herbert Irving Comprehensive Cancer Center in New York City, and her colleagues have been studying more than 1,300 people with breast, ovarian or non-small cell lung cancer to learn more about who develops CIPN and what factors might affect this chemotherapy side effect. Their long-term goal is to develop a clinical risk prediction model to help doctors make treatment decisions with their patients. The study is looking at patient-reported experiences of neuropathy, type of chemotherapy used and dose changes over the course of treatment, along with factors like activity levels. So far, more than 90% of study participants have been breast cancer patients. Two-thirds of those breast cancer patients reported clinically meaningful neuropathy at some point during the first year of the study, and nearly half of patients reported neuropathy that persisted at the one-year mark.
At the 2023 ASCO Annual Meeting in Chicago, Trivedi and her colleagues presented preliminary results that compared two taxane chemotherapies, paclitaxel and docetaxel, both important in breast cancer treatment. The researchers evaluated 1,103 breast cancer patients at regular intervals. Over 24 weeks, people who received paclitaxel consistently had more neuropathy symptoms than those who received docetaxel, the researchers found.
“We’re hoping that studies like this one that help better characterize and understand the physiology of CIPN will help us create better prevention and treatment modalities,” Trivedi says. “I think the most important takeaway is to understand that we need to be assessing our patients for this frequently and making sure that we make the appropriate adjustments to their treatments as we can.”
Reducing Symptoms
Along with adjusting the types and doses of chemotherapy treatments, several strategies have shown promise in easing neuropathy symptoms in some patients. An analysis published Aug. 1, 2023, in JAMA Network Open looked at the effect of exercise on CIPN in a clinical trial of 134 people with ovarian cancer. Those who participated in an at-home aerobic exercise program for six months reported significant improvements to their neuropathy symptoms, compared with those who did not participate.
While the evidence is not yet sufficient to include exercise in the official treatment guidelines for peripheral neuropathy, Loprinzi says, “there is a suggestion that exercise can be helpful for preventing and/or treating neuropathy,” along with having many other health benefits.
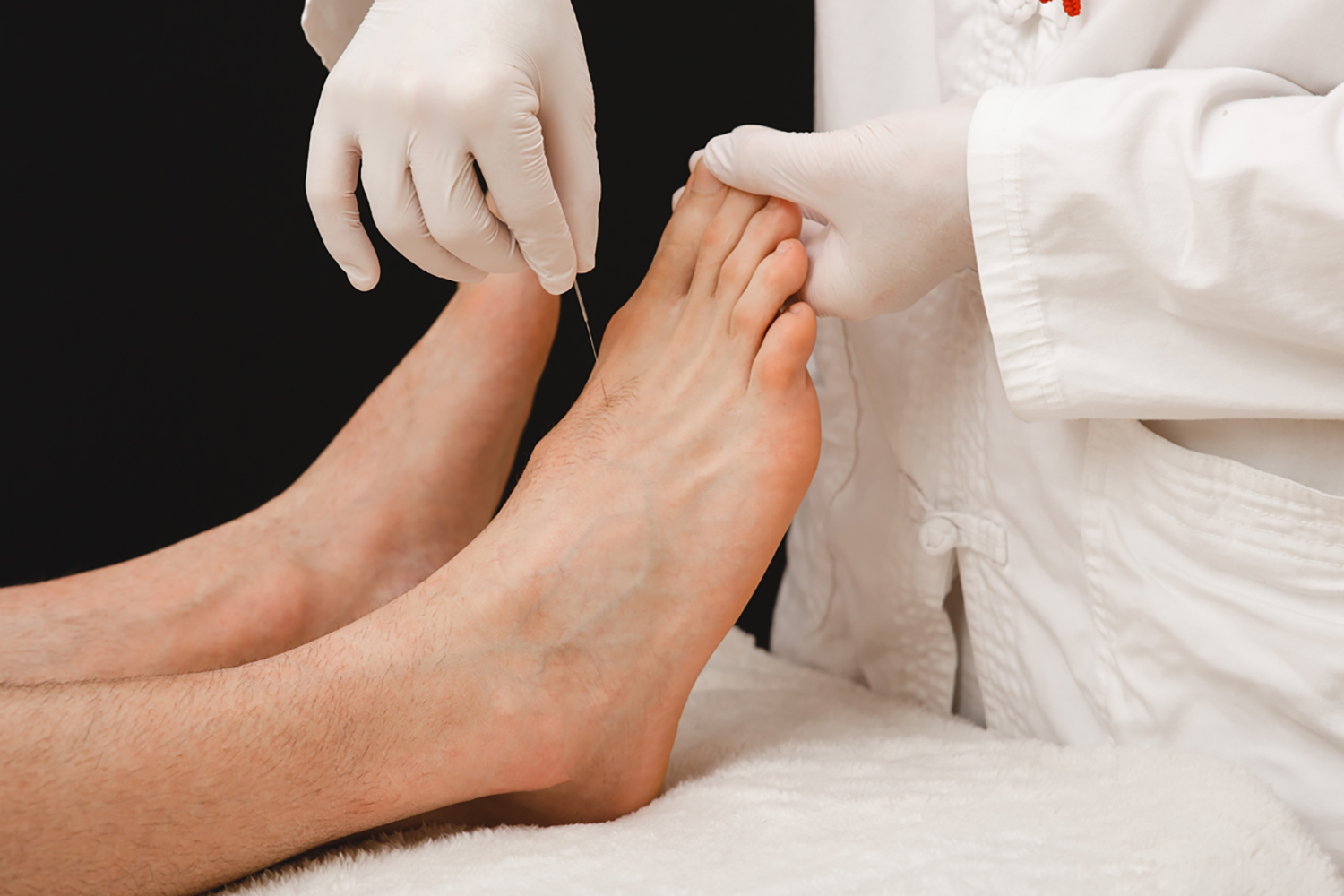
Photo by Peakstock / Shutterstock.com
Another approach to treating neuropathy symptoms is acupuncture, which Oehler’s doctor recommended when her peripheral neuropathy worsened. Acupuncture, a practice based in traditional Chinese medicine, involves very thin needles placed at different points on the body. At first, Oehler was unsure about the treatment, but with the encouragement of her oncologist and a medical acupuncturist at the Nassif Community Cancer Center in Cedar Rapids, she started receiving acupuncture every seven to 10 days and continued for a period of two months. She began to look forward to the half-hour sessions spent with peaceful music playing in the background, and her neuropathy symptoms began to ease. “After about two weeks, I noticed a big change,” she says.
A 2019 review in Current Oncology evaluating three clinical trials involving 203 patients with CIPN found that two of the three trials indicated acupuncture helped with CIPN pain, while one showed no benefit. The review concluded that more research is needed to evaluate the effects of acupuncture on CIPN. On March 11, 2020, researchers from Memorial Sloan Kettering Cancer Center in New York City published in JAMA Network Open results from a clinical trial that followed 68 people with solid tumors who had moderate to severe CIPN. Researchers found that eight weeks of acupuncture was most effective at reducing pain levels, based on patients’ rating of pain on a numeric scale, compared with standard treatments and “sham” acupuncture (a comparison technique that mimics the acupuncture sensation but does not use needles or acupuncture points). Researchers are now conducting more extensive clinical trials. “Acupuncture is one of these interventions that really is low risk, but it may help,” Trivedi says.
New research seeks to learn about the effects of acupuncture as a tool to manage peripheral neuropathy.
Acupuncture, a traditional practice rooted in Chinese medicine, has been shown to help in treating painful conditions, including back, knee and headache pain. When it comes to addressing peripheral neuropathy after cancer treatments, “we’re earlier in the evaluation process,” says Heather Greenlee, the medical director of the Integrative Medicine program at Fred Hutchinson Cancer Center in Seattle.
Greenlee has already been working to learn more about the role of acupuncture in easing other side effects of cancer treatment. In 2018, Greenlee and her colleagues published findings in JAMA from a large, randomized clinical trial on acupuncture that looked at 226 people with breast cancer from 11 cancer centers. The study found acupuncture reduced joint pain associated with aromatase inhibitors, which are given to lower estrogen levels and reduce the chance of breast cancer recurrence. Greenlee says she has seen the benefit of acupuncture for chemotherapy-induced peripheral neuropathy (CIPN) in the clinic. “But we want to understand how to optimize it,” she says.
Now, a team at Fred Hutchinson Cancer Center is working on a phase II clinical trial looking at just that in patients with gastrointestinal cancers. The trial is comparing a combination of acupuncture plus acupressure to oral cryotherapy—using ice chips or other cold treatments in the mouth, which in other studies has been linked to improved chemotherapy side effects, including decreased peripheral neuropathy.
For patients, one challenge is that not all health insurance plans cover these supportive treatments that are currently not part of many clinical guidelines or standards of care, Greenlee says. “We’re conducting this research to accrete a large enough body of evidence to determine if acupuncture is effective in improving CIPN,” she says, which could make acupuncture and other supportive treatments more available.
Pain Is a Priority
As an oncologist and palliative care expert, Thomas J. Smith says the worst pain he sees in his patients with breast cancer is CIPN—and he sees how pain affects everything from the patient’s family to the patient’s survival. Smith, the director of palliative care at Johns Hopkins Medicine in Baltimore, has tested an approach to treating peripheral neuropathy pain called scrambler therapy, approved to treat pain by the Food and Drug Administration in 2009. Scrambler therapy is a form of noninvasive electrical stimulation. Providers place electrodes on the skin above and below the place where a person is feeling pain. In 2010, Smith and his colleagues published results from one of the first pilot trials of scrambler therapy for CIPN in the Journal of Pain and Symptom Management, which found that 15 out of 16 cancer patients had their pain reduced by 20% or more on a numerical pain scale. “Some patients had their pain go to zero,” says Smith, who at first was skeptical of the therapy’s potential.
In a review published July 13, 2023, in the New England Journal of Medicine, Smith and his colleagues looked at multiple clinical trials of scrambler therapy and found that it may help with pain in 80% to 90% of patients. “Speaking as a survivor, you’ve already had your life turned upside down several times. The last thing you need is this persistent pain,” he says. Relieving pain “can dramatically change people’s lives.”
Preventing Symptoms
Loprinzi, at Mayo Clinic, has spent most of his career running clinical trials to address the side effects of cancer treatment. When it comes to CIPN, he is most encouraged by clinical trials using cold and compression therapy, not just to help with symptoms but to prevent CIPN from happening in the first place. Cold therapy, or cryotherapy, was first developed to prevent hair loss during chemotherapy, but a 2013 study of 1,725 patients in Breast Cancer Research and Treatment suggested that patients who wore frozen gloves and socks during chemotherapy were less likely to develop peripheral neuropathy.
Subsequent clinical trials have looked at both cold therapy and compression therapy, which involves compressing the feet and hands with elastic stockings, surgical gloves and other devices. Loprinzi says both methods may work in a similar way, by restricting blood flow to the extremities. He and his colleagues recently launched a new clinical trial that will look at several approaches to prevent CIPN. The trial will have groups of cancer patients receiving either compression therapy or a combination of cold and compression therapy, along with a control group receiving neither therapy, to better understand which approach is most effective in preventing CIPN.
Christine Hodgdon, who was diagnosed with metastatic breast cancer in 2015, participated in a clinical trial looking at cryotherapy while receiving paclitaxel as part of her chemotherapy regimen. She wore frozen gloves and booties on her hands and feet during treatment. As soon as her body heat started warming up the gloves and booties, her medical team would switch them out for a new, frozen pair. “Slight discomfort, but worth it because I have very little neuropathy,” says Hodgdon, the co-founder of GRASP, a cancer advocacy organization connecting patients and researchers.
Hodgdon encourages those with CIPN—and those concerned about developing this and other chemotherapy side effects—to look into clinical trials aimed at prevention and treatment of side effects, as well as those looking at treating the cancer itself. More patients participating in trials “means more data collected, and faster research advances that can provide interventions that reduce the burden of symptoms and side effects for patients,” Hodgdon says.
Talk About It
Trivedi encourages people to talk with their health care providers if they start experiencing neuropathy symptoms in their hands or feet during chemotherapy. “If someone doesn’t tell us, we don’t know what they’re experiencing,” she says. With more understanding of how a patient is faring during and after chemotherapy, “we can try and help the symptoms that are associated with the therapies.”
Oehler also suggests being honest with your health care providers about the extent of your symptoms so they can try to find solutions. “As a younger person, I felt a little embarrassed to say that I was tripping on stuff and falling,” says Oehler, who was diagnosed when she was 48.
In her case, stepping out of her comfort zone, both to talk with her doctor about CIPN and to try acupuncture, helped her feel better, eventually allowing Oehler to return to her regular activity levels and her dressy shoes. “You just want to feel as normal as you possibly can post-diagnosis,” she says. “I was very thankful.”
Cancer Today magazine is free to cancer patients, survivors and caregivers who live in the U.S. Subscribe here to receive four issues per year.