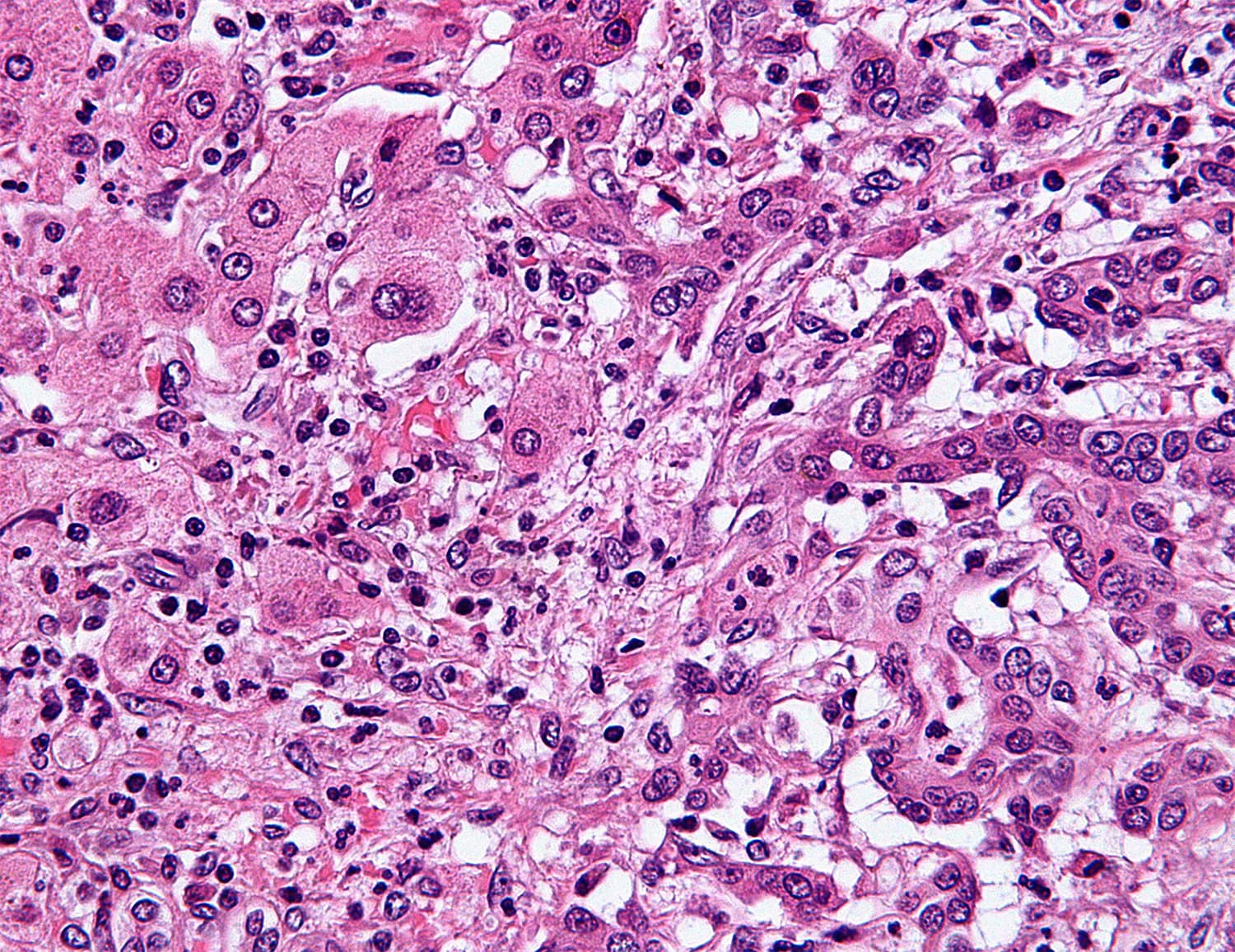
Targeted Therapy for Bile Duct Cancer
Bile duct cancer, also called cholangiocarcinoma, is a rare cancer with a five-year survival rate under 20%. Chemotherapy and surgery have been the main treatments available, but a fraction of patients with this type of cancer may respond to targeted therapies. A study published Aug. 17 in the Lancet Oncology finds that for the approximately 5% of people with biliary tract tumors who have a BRAF mutation, treatment with a combination of Tafinlar (dabrafenib) and Mekinist (trametinib) may be an option. The combination has already been approved for treatment of some patients with melanoma, non-small cell lung cancer and anaplastic thyroid cancer. Researchers studied Tafinlar and Mekinist in 43 patients with biliary tract cancers with a BRAF V600E mutation who had undergone prior treatment and found that the targeted drugs shrunk the cancers in about half the participants. Median overall survival for the participants was 13.5 months, and seven patients still had a response to the therapy after a year. Lead author Vivek Subbiah of the University of Texas MD Anderson Cancer Center in Houston told Targeted Oncology that genomic testing should be made available to patients with bile duct cancer, not just for the BRAF mutation but for other molecular alterations that may provide additional treatment avenues. “For an oncologist, especially treating bile disease, my personal opinion is that universal genomic testing should be the message to win the war against cancer,” he said.
The Patient Perspective on Hormone Therapy
People with hormone receptor-positive breast cancer are often prescribed hormone therapy. But many patients do not stay on these drugs, which include tamoxifen and aromatase inhibitors, for the full recommended period. Results from a survey of people with breast cancer published Aug. 17 in the Journal of Cancer Survivorship explored the various reasons people do not take the medications. The survey was created by nine patient advocates and eight medical experts and distributed via social media, an e-newsletter and a blog post. The researchers analyzed responses from 2,353 women and 54 men who took hormone therapy for breast cancer. They found that 92% of women and 74% of men experienced side effects. The most common side effects for women were musculoskeletal issues and general physical changes like weight gain and problems with body image. Men were most likely to report sexual side effects and problems with cognition or mood. Men with metastatic breast cancer were also likely to report musculoskeletal issues. Around one-third of women and half of men stopped taking their hormone therapy early, and 32% of participants said they felt their care team dismissed or minimized their concerns about side effects. Finally, most of the participants appeared to understand the purpose of their treatment, but this was not associated with higher likelihood of remaining on the therapies. “This suggests that understanding of the importance of therapy may not be sufficient for adherence when patients face medication-related side effects that significantly interfere with quality of life,” the authors write.
More Data on Chemotherapy and COVID-19
Receiving chemotherapy may not put cancer patients at increased risk of severe or critical COVID-19, according to a study published Aug. 14 in the Journal of Clinical Oncology. Researchers at Memorial Sloan Kettering Cancer Center in New York City analyzed data from 309 patients who were diagnosed with COVID-19 in March 2020. They found that recent chemotherapy treatment, delivered with 14, 35 or 90 days of a COVID-19 diagnosis, was not associated with severe or critical COVID-19. Some previous studies did show a link between recent chemotherapy and severe COVID-19, but larger registry studies did not find this connection. The researchers note that their new study does not rule out the possibility that chemotherapy could increase risk of severe COVID-19 for subsets of patients, depending on factors like cancer type or race. The researchers also found that patients with lung cancer or blood cancer were at increased risk of severe or critical COVID-19.
Cancer Today magazine is free to cancer patients, survivors and caregivers who live in the U.S. Subscribe here to receive four issues per year.