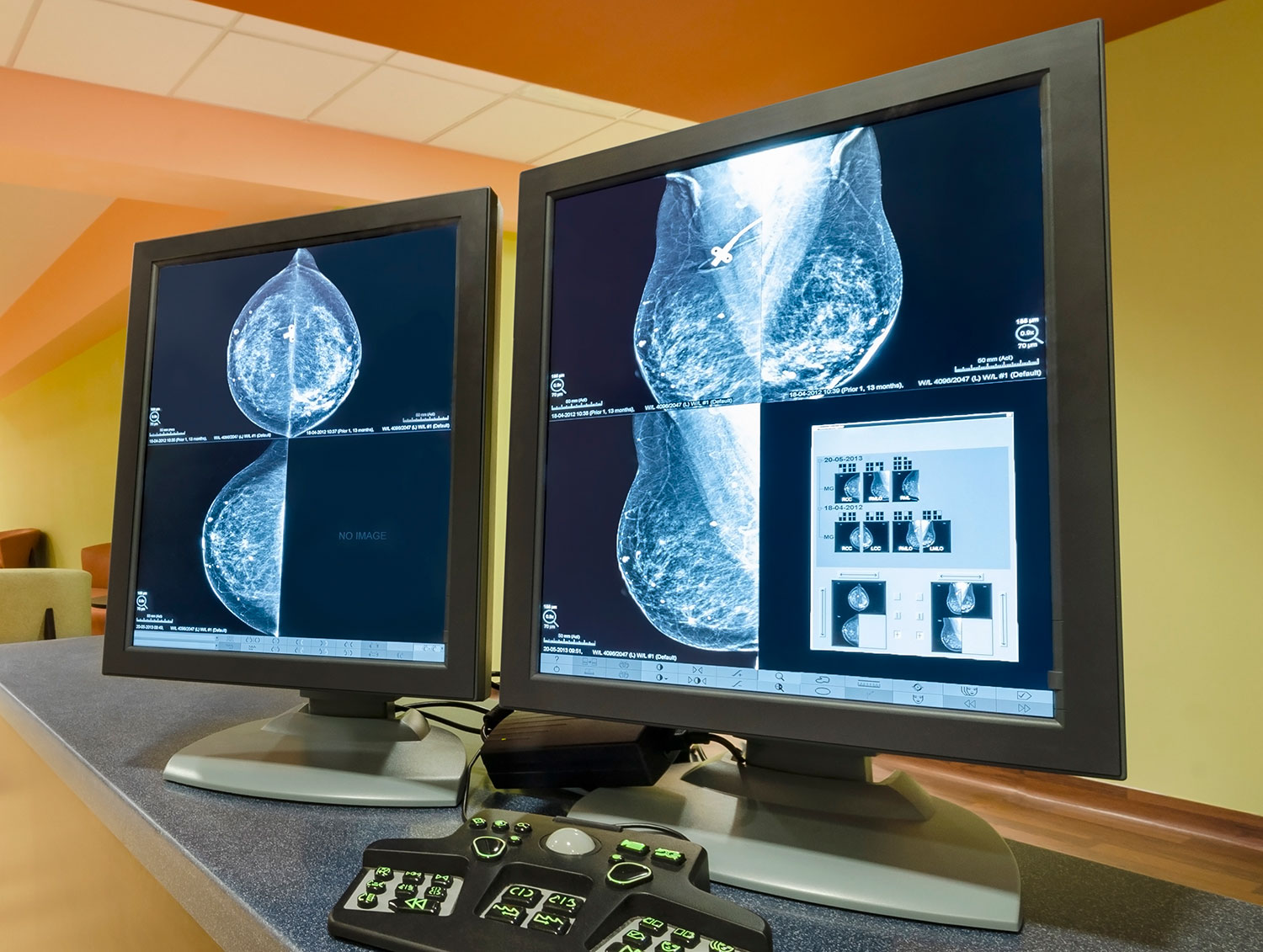
Using Artificial Intelligence to Read Mammograms
An artificial intelligence system was able to interpret mammograms with fewer false-negative and false-positive results than radiologists, according to a study published Jan. 1 in Nature. Researchers trained the algorithm using mammograms from women in the U.S. and U.K. and then tested it on mammograms from a separate set of women from these countries. The algorithm yielded 9.4% fewer false-negative results than radiologists in the U.S. and 5.7% fewer false-positive results. It yielded just 1.2% fewer false-positive results and 2.7% false-negative results than radiologists in the U.K., where women receive mammograms less often and have them examined by two rather than one radiologist, according to the Guardian. Study co-author Shravya Shetty of Google Health in Palo Alto, California, told the Verge that the algorithm, which is not yet ready for clinical use, is intended to supplement rather than replace the work of radiologists. “There are a number of cases where the radiologists catch something that the model misses, and vice versa,” Shetty said. “Bringing the two together could strengthen the overall results.”
A Year of Cancer Misinformation
Misinformation about health can spread rapidly via the internet. In an article published Dec. 29, NBC News analyzed the spread of articles about health on social media, identifying the most viral health misinformation of 2019. “Overall, cancer was the subject of the most popular kind of health misinformation, with viral articles promoting unproven cures for cancer making up roughly a third of our list,” writes reporter Brandy Zadrozny. The article on cancer that got the most engagement claimed that “Big Pharma” was hiding a cure for cancer and was from a site that was banned from Facebook in June 2019 due to “misleading or inaccurate” posts.
Life After Pediatric Cancer
Improvements in cancer treatment have raised the five-year survival rate for children diagnosed with cancer. Today, 80% of children diagnosed with cancer live five years or more following their diagnosis. But treatment for pediatric cancer can come with long-term problems, like second cancers and heart disease. In a study published Jan. 2 in JAMA Oncology, researchers used a model to calculate the expected lifespan of children diagnosed with cancer in different decades. They estimated that people diagnosed with pediatric cancer in the 1970s have a 25% shorter life expectancy than people without a history of cancer and that those diagnosed in the 1990s have a 14% shorter life expectancy. Patients treated with just chemotherapy saw the greatest improvements in life expectancy between the 1970s and 1990s. Patients treated with radiation or radiation plus chemotherapy had more modest life expectancy improvements. The percentage of pediatric cancer patients treated with chemotherapy alone rose from 18% in the 1970s to 54% in the 1990s. “Our findings emphasize the importance for survivors to adhere to follow-up care and risk reduction behaviors because subsequent primary cancers and cardiac events were the leading causes of early mortality in all subgroups,” the researchers write.
Targeted Therapy for Pancreatic Cancer
A class of targeted therapies called PARP inhibitors can be used to treat certain cancers that have flaws in DNA repair. The U.S. Food and Drug Administration on Dec. 27 approved the PARP inhibitor Lynparza (olaparib) for treatment of patients with metastatic pancreatic cancer who have hereditary BRCA mutations. The treatment is intended for patients whose cancers have not grown or spread during platinum-based chemotherapy. Lynparza and other PARP inhibitors previously have been approved for treatment of some patients with breast and ovarian cancer. This is the first time a PARP inhibitor has been approved for treatment of pancreatic cancer.
Cancer Today magazine is free to cancer patients, survivors and caregivers who live in the U.S. Subscribe here to receive four issues per year.